Wyszukaj w wideo
Jak za pomocą rezonansu magnetycznego serca możemy zdiagnozować zespół zapalenia mięśnia sercowego i osierdzia, a kiedy to jest za mało?
III Międzynarodowy Kongres Kardiomiopatii
III Międzynarodowy Kongres Kardiomiopatii to jedno z najważniejszych wydarzeń w kalendarium osób zajmujących się chorobami sercowo-naczyniowymi. Podczas edycji 2026 odbyły się sesje dot. choroby Fabry’ego, zapaleń mięśnia sercowego, chorób osierdzia, HCM, amyloidozy i diagnostyki obrazowej.
Odcinek 29
Ostatni wykład, „Jak za pomocą rezonansu magnetycznego serca możemy zdiagnozować zespół zapalenia mięśnia sercowego i osierdzia, a kiedy to jest za mało?”, wygłoszony przed Annę Baritussio, MD, PhD z Uniwersytetu w Padwie, również nawiązywał do szeroko dyskutowanego podczas paneli dyskusyjnych tematu: możliwości zastąpienia biopsji endomiokardialnej przez MRI.
[outro jingle] Uh, good evening, everyone.Thank you very much forthe, um, invitation.Uh, tonight we're going totalk about the role of CMRin this new umbrella termthat has been introduced with the,um, latest guidelines last year,that is the, um, uh, inflammatorymyopathic cardiac syndromes.Uh, in these cases, CMRhas definitely a diagnostic role becausewe' see, um, the abilityof CMR to, uh, provide tissuecharacterization is really very muchsupportive of the diagnosis.And although I won't touch,uh, on this tonight, uh, CMRhas an important role al-alsofor prognosis in these, uh, uh,in these patients.
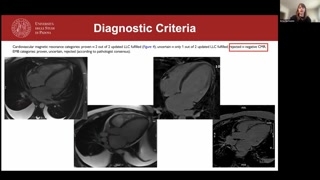
Um, as you see, theflow chart, uh, uh, from thelatest guidelines, uh, is theone I'm showing here.If we have, uh, aclinical presentation that is suggestive formyocarditis, we have a first-lineassessment with physical examination, ECG, echo,lab assessment.We need to rule outcoronary artery disease.That's a condition, uh, sinequa non, uh, to, uh, providethe diagnosis of myocarditis.And, uh, if the patientdoes not have high-risk clinical features,that is, um, uh, uncontrolled,uh, ventricular arrhythmias, uh, cardiogenic shock,unresponsive, um, um, r-heart failure,uh, the, um, indication is topr- to perform a CMR.You see here is aclass one recommendation to get towhat is being drawn asa pyramid with a possible definiteor rejected diagnosis.And as you see herefrom the new guidelines, a definitediagnosis can be achieved witha feasible clinical presentation along witha consistent CMR or aconsistent EMB.Not both, but one orthe other, and we may discussabout this later.
So, uh, we have someimaging criteria, some CMR criteria thatare the new or updatedLake Louise criteria, uh, that havebeen, uh, upgraded.The previous, uh, Lake Louisecriteria that were based basically onthe presence of edema orhyperemia or necrosis, we needed twoout of three.But the new, uh, LakeLouise criteria require a T2 criteriafor the evidence of myocardialedema and a T1 criterion, uh,for, uh, the evidence ofnon-ischemic myocardial injury, along with supportedcriteria, which have been, uh,unchanged since the previous, um, criteria,that are the presence ofleft ventricular systolic dysfunction and, uh,the evidence of pericardial involvementby means of pericardial edema or,um, pericardial effusion.
Uh, when it comes tothe T2 criterion for myocardial edema,we may use the standardT2 weighted sequences where myocardial edemaappears as a hyperintense, uh,signal, as you see here shownby the arrows.Uh, the, uh, typical, uh,edema in myocarditis patients has aknown ischemic pattern, which meansthat the subendocardium is spared andthe edema involves the subepicardiumor the mid-wall, and it doesnot follow, uh, the distributionterritory of a coronary, um, uh,artery.
Um, of course, timing isvery important because edema may resolveover time.So if we scan thepatient too late, we may havenegative T2 images, not becausethe patient does not have myocarditis,but because we've waited toolong to perform the scan.But on the other hand,also too early may be wrong,because if we scan tooearly, we may not have, uh,evidence yet, uh, of, uh,edema on T2 weighted imaging.
So timing is really very,very much important.Um, we may also usefor our T2 criterion, not justthe standard T2 weighted sequences,but the, uh, T2 mapping.T2 mapping is a parametricmapping that provides some maps thatbasically refle-reflect how healthy orhow unhealthy the, um, myocardium is.And in our lab, yousee the normal myocardium on T2mapping appears as a purple-pinkish,uh, color, and the more edematousthe myocardium is, so thehigher the T2 values, the moreyellowish the myocardium will be,as you see here in, inthis case.
It's always very, very importantto know and to provide thereference values for T2 mappingin your lab, in your scan.Because you see here, ifthe reference value is below forty-fivemilliseconds, you do understand thathaving T2 values greater than ahundred, this really means thatthere is a lot of, uh,edema.And also you can appreciateit h-here also visually because thenormal myocardium left is justthis, uh, little portion of thebasal and m-mid cavity, uh,infraseptum.
But we also need, wesaid, a T1 criterion that, uh,um, in-- represents, uh, non-ischemicmyocardial injury, and we may usestandard post-contrast sequences to lookfor late enhancement.Late enhancement will have aknown ischemic pattern in myocarditis patients.So once again, it willspare the subendocardium and have asubepicardial or, um, mid-wall, um,distribution that does not follow, uh,uh, a coronary artery distributionpattern as you see, uh, verywell in this case hereon the right side, uh, ofthe screen.
But we may also use,uh, T1 mapping, um, to, uh,look for, uh, signs ofa myocardial inflammation by using nativeT1 mapping, which is performed-Priorto the administration of contrast.Again, native T1 map inour lab, uh, as, uh, showsthe myocar-- normal myocardium asa purple, um, color.And the more abnormal themyocardium here is, the higher thenative T1 mapping will bein myocarditis and the more orange-ish,uh, the signal will be.And it's, again, very muchimportant that you provide the normalvalues in your lab.So you see here wehave, uh, eleven hundred, uh, millisecondswhen it is normal, upto one thousand and forty milliseconds.
If we perform the T1mapping before and after contrast administration,we can get another mapthat basically measures and quantifies the,uh, extracellular volume, the, uh,interstitial space, and you do knowthat ECV, uh, is avery important ma-marker, especially when itcomes to prognoses in differentcardiomyopathies.And here again, it's veryimportant to have the normal, uh,references, and in our lab,it's, uh, normal up until thirtypercent.
So to show you somecases, this is a fifty-five-year-old malewith hypertension, dyslipidemia, obesity.He had no family historyof heart disease, and he presentedbecause of palpitations.He was prescribed an exercisetesting, and he had ventricular arrhythmiason effort.An echo was m-barely normal,only showing a mildly dilated leftventricle with, with preserved function,and therefore we performed, um, CMR.Coronaries were, of course, uh,normal on angiogram.
So as you see here,we have, uh, a mildly dilatedleft ventricle with a borderlinelow normal ejection fraction because ofsome regional wall motion abnormalitieshere in the anterolateral mid wall.
And when we look atparametric mapping, what we see isthat we have a mildincrease in T2 values compared towhat is normal in ourlab, and it's mainly abnormal herein the, um, posterior wall.Uh, we also have increasednative T1 values.As you see here, wehave eleven hundred as compared tothe one thousand and forty,which is the upper range ofnormal in our lab.And we also have anincrease in the extracellular volume, whichis above the th-thirty percentthat is the upper range ofnormal in our lab.
If we perform late enhancementsequences, normal myocardium appears black, andlate enhancement is a brightsignal.Uh, you see that wehave quite a lot of lateenhancement, mainly in the basallateral wall, as confirmed both onthe long-axis and the short-axissequences, but we also have somemid-wall, uh, involvement of thebasal septum.So here we have anon-ischemic late enhancement, uh, because yousee here the subendocardium isspared, and it's a mid-wall distribution.
Uh, so we can concludethe patient has, uh, myocardial inflammation,acute myocardial inflammation because wehave the T2 criterion, as shownby the T2 mapping, andthe T1 criterion of m- non-ischemicmyocardial injury, as shown bythe, by the non-ischemic, um, LGof the left ventricle andthe increased native T1 and ECV,uh, values.
This is another case ofa sixty-one-year-old male, ex-smoker.He presented, uh, urgently, uh,with, um, abdominal pain.He underwent surgery.Post-surgery, he had paroxysmal atrialfibrillation with markedly increased, uh, troponinvalues, normal, uh, coronary arteries,uh, but with a moderate LVdysfunction.
So what is the reasonof the increased troponin levels?So we perform CMR, andas you see here from theCV sequences, we confirm themoderate dysfunction.But you do see thatthere is some regional wall motionabnormality that, that is, um,concentrated and localized to the midportion of the left ventricle,while the apex and the basecontracts normally.
And if we look atparametric mapping, we see that T2values are markedly increased.You see that overall itis more orange-ish than the purplethat we would expect inour lab.And also T1, native T1values are quite increased, as yousee once again by thisorange-ish appearance of the myocardium thatusually appears purple in ourscanner.And when we go tothe extracellular, um, volume quantification that,uh, I remind you inour lab, uh, uh, the upperrange of normal is thirtypercent, you see here that theextracellular volume is markedly increased.It's more than twice, uh,the upper range, uh, of normal,uh, in our scanner.
And if we look atlate gadolinium enhancement, you see herewe have quite extensive lateenhancement, especially if you look atthe short axis.You see it's almost circumferential,and it's almost base to apex.It has a known ischemicdistribution pattern because the subendocardium is,um, is spared.So it's mainly a mid-walldistribution.
So here we have apatient with left ventricular dysfunction, markedlyincreased T2 values, so wehave our T2 criteria, markedly increasednative T1, ECV values withextensive late enhancement.So this is definitely, uh,a known, uh, ischemic cardiomyopathy, butwe can call it basedon Lake Louis criteria, um, inflammatorycardiomyopathy.
And this patient underwent endomyocardialbiopsy with-which confirmed the diagnosis ofa lymphocytic, uh, virus negativemyocarditis.
I' show you also anothercase.This is a fifty-two-year-old malewith no risk factors, no cardiovascularrisk factors.He had, um, a paroxysmalatrioventricular block, normal echo, normal coronaries,so he was implanted witha pacemaker.And a few months later,he developed a cardiac arrest, andon checking his pacemaker, wefound loads of non-sustained VTs andalso the VTs that caused,uh, the cardiac arrest.Echo was really not thatremarkable because he had normal, um,left ventricular, uh, ejection fraction,although there was mild left ventricularhypertrophy, but the right ventriclewas mildly dilated and dysfunctional.So what is the causeof the cardiac arrest and theabnormal, uh, right ventricle onecho?
So we performed CMR.As you see here, wehave the native T1, uh, theT2 mappings, and you seehere we have our normal myocardiumthat should be purple, butyou see here the hypertrophied septumthat has increased values.Although I don't put thenumber here, I know they areincreased because you see herepurple is normal, and the highertheT1 values, the more orange-ishor yellowish, uh, the, uh, colorof the map.And the same applies toT2 mapping.It should be, uh, wesaid purple pinkish, but if wehave increased T2 values, wewill have more orange-ish, um, uh,color.And you see here thatin the septum exactly where wehave increased T1 maps, wehave, uh, increased T2 mapping values.And these coincides with areasof myocardial edema on standard T2weighted images.And here you see onthe septum that we have aknown ischemic, um, edema ofthe, uh, basal anteroseptum, uh, as,um, a edematous stria thatinvolves the subepicardium.
So if we look atdelayed enhancement sequences, what we appreciatehere is that we havequite extensive late enhancement that mainlyinvolves the septum with aknown ischemic pattern.You see that the, uh,subendocardium is spared.This LGE of the septumextends to the adjacent, uh, anteriorand inferior walls, but wealso have late enhancement of theright ventricle.So we have extensive non-ischemicbiventricular LGE in patients that alsohas evidence of myocardial edemaand has a particular history ofbrady and tachy arrhythmias.
So we had a specificsuspicion in our head, but weneeded confirmation.And what we did wasto perform a PET scan becauseour suspicion was of asarcoid.And the PET scan allowedus to confirm the, uh, involvementof the heart, as yousee here from the images, butalso that there were areasoutside the heart that showed increasedmetabolic activity.We could, uh, biopsy theseareas easily.
So we can use thePET to look for areas thatare more easy to biopsy.We perf- we confirm thediagnosis of sarcoid in the liver.And so by having anextra cardiac histological confirmation of sarcoidosisalong with a CMR anda PA- PET scan that areconsistent with cardiac involvement fromsarcoidosis, we could confirm the diagnosisof a systemic sarcoidosis withcardiac involvement.
So very, very nice.Uh, CMR is very useful.Uh, we do know thatthe recent guidelines do say ifyou have either EMB orCMR that are consistent with myocarditisin a proper clinical picture,you have a definite diagnosis.
Uh, but sometimes it happens,for example, that CMR is uncertainbecause maybe we scan tooearly and we only have oneof the two criterion, sothe diagnosis may be possible.But I want to putyour attention to the rejected diagnosisbecause what the guidelines sayis that if nega- if CMRis negative, there is nomyocarditis.
And I want to showyou that it's not always thiscase because this, you seehere, this is a patient with,um, heart failure presentation, veryyoung patient, normal coronaries.Uh, she had, as yousee here from these images, uh,severe biventricular, um, dysfunction thatwas not really very much responsiveto treatment.As you see on lateenhancement, there was little, if no,uh, late enhancement.So the scan, the CMRscan was, um, uh, was, um,considered consistent with a DCM.But, uh, clinically, we hadan indication for EMB, and wewere, uh, lucky to dothat because, uh, endomyocardial biopsy confirmedthe diagnosis of a activelymphocytic virus negative myocarditis.And the patient could undergo,uh, immune suppressive treatment and, um,she recovered, uh, progressively almostto a normal, um, ejection fraction.
So we have to bearin mind that although Lake Louisecriteria are very good, uh,only a minority of studies, um,included histologically proven myocarditis.And this is very importantbecause although we do know thatin myocarditis with infarct-like presentation,the accuracy of CMR is veryhigh for diagnosis.When it comes to otherpresentations, specifically the heart failure andthe arrhythmia presentation, the accuracy,diagnostic accuracy of CMR, uh, fallsquite significantly.
And this is because patientsthat have this cardiomyopathy-like presentation havea longer disease course beforegetting to the medical attention.So there's a long timespan where water reabsorbs, so wedo not see edema anymoreon T2 weighted sequences because theyhave lower sensitivity.And also there's a prevalenceof apoptosis rather than necrosis inthese stages.And we do know thatlate enhancement cannot cross, um, cellmembranes that are intact.So we do see gadoliniumlate enhancement where we have necrosis,but if we have apoptosisas a predominant, uh, mechanism ofcell death, we may havenegative LGE sequences.
So we need to bearthis in mind that especially cardiomyopathy-likepresentation may have negative CMR.So we need to havea high suspicion and request furthertesting also if the CMRis negative.
Mapping may be promising becauseit has been shown that especiallyin the cardiomyopathy group, itmay increase diagnostic accuracy, but it'salways very important that weprovide or pretend to have thenormal values for mapping inthe scanner because if you onlyhave a slight increase ora significant increase, it makes alot of difference clinically.
Another point I want toraise is that, uh, we dosay that CMR is verygood for differential diagnosis in cardiomyopathy.And as you see herein these two examples of apicalhypertrophy, CMR is very usefulbecause by using late enhancement sequences,we distinguish two complete differentdiseases.On one hand, apical HCM,on the other hand, eosinophilic myocarditis.
But it is not alwaysthat easy because I want toshow you here these cases,two cases.We have in both casesextensive non-ischemic late enhancement with, um,significant involvement of the septumand onlyEndomyocardial biopsy can label thesetwo diseases that are verydifferent.On one hand, we havea lymphocytic myocarditis, on the otherhand, we have sarcoidosis.So it's a s- tremendous,um, technique, but it has somelimitations that we need tobe aware of.
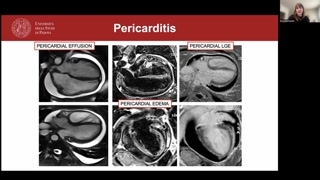
When it comes to pericarditis,I have to be honest withyou, I think it's aclinical diagnosis.I would be very puzzledif we needed to use CMRto get to the diagnosis.But sometimes we may seesome pericardial involvement, uh, by meansof pericardial edema or lateenhancement, for example, in patients withmyocarditis.Anyway, if you cannot cometo a diagnosis clinically or notsure for whatever reason, CMRis recommended as a class oneby the latest guidelines.
Why is that so?Because basically we can,use tissue characterization to, um, lookat the pericardium as well,because we may see thickness ofthe pericardium, but mainly edema,and so the presence of inflammationand the presence of lateenhancement.It, it does not alwaysmean, um, uh, fibrosis because ifwe have, uh, inflammation ofthe pericardium, we may have, uh,increased vascularization.And so if we haveincreased vascularization, there is where thelate enhan- the gadolinium willgo.So we may have lateenhancement as, um, um, sort of...Meaning, uh, myocardial, uh, pericardialedema rather than, uh, fibrosis.
Um, how does pericarditis looklike on CMR?It's very easy.We may see the presenceof pericardial effusion, as you seehere in this, um, severe,um, effusion, uh, that is circumferential.But if we have anacute pericarditis, we will expect tosee pericardial edema that veryeasily will look as a hyperintensesignal on the pericardium, whichwe c- you can clearly seehere because it's also verymuch thickened, and this makes thingsmuch easier.And also we will havelate enhancement, as you see here.
Um, the pericardium should appearas a low-intensity structure in allsequences in CMR, so alsoon the late enhancement.So if we see ahyperintense, uh, or an, uh, or,uh, enhanced, uh, pericardium, uh,on late enhance- on late enhancementimages, that means that wehave late enhancement.But as we said previously,this does not necessarily mean thatthere is fibrosis as somechronicity marker.But, uh, if we haveincreased inflammation, increased vascularization, we maysee, uh, late enhancement asa meaning of active inflammation.
Uh, of course, although echois the best to assess physiology,we may use real-time cinesequences and acquire cine sequences ofthe heart with the patientbreathing, uh, freely.And you can appreciate theabnormal motion of the septum, whichis specific of constriction.
But what I wanna showyou is that, um, is asituation where CMR is reallyvery useful, and it's a caseof an eighteen-year-old male.He presented with syncope, uh,following a few months of chestpain that was consistent withpericarditis.He also had quite increased,uh, CRP values, as you seehere.And his echo showed asevere circumferential organized, uh, effusion witha very thickened pericardium.But what is interesting isthat when looking at physiology, wefound signs of constriction.What is important to knowis up to twenty, thirty percentof cases have a constrictivephase in the acute phase ofpericarditis because the edematous pericardiumis, um, constrained and it constrainsthe heart.It cannot relax much.So it is not uncommonto find constriction in early phasesof acute pericarditis, and thisis usually reversible, and that's whyguidelines say you have totreat these patients with proper, uh,anti-inflammatory, um, therapy, and youneed to check the patient becauseusually this case, uh, revert,uh, after appropriate treatment.
And in these cases, CMRis very useful.Why?Because if we have acute,um, if the constriction is dueto acute inflammation, I'm expectingto see something at the pericardiallevel.And this is the caseof the patient, where you canappreciate that we have herethis, uh, effusion that is organized.But as you see onthe T2-weighted images, we have quitea lot of pericardial edemaas well as quite a lotof late enhancement is this,in this thickened pericardium.And this late enhancement isnot m- a sign of chronicfibrosis that means we haveto call, uh, the surgeon becausethe patient has chronic constriction.But this is a s-a sign of acute pericardial inflammationthat explains the, um, constrictivephase.So this means we needto treat the patient, we needto keep with the treatmentuntil the acute inflammation resolves.
So to wrap up, uh,I hope I've shown you thatCMR has a complementary rolein the diagnosis of inflammatory myopericardialsyndromes.Timing is very much important,so it's really very important thatyou, uh, choose the rightwindow to scan your patients.CMR is tremendous for diagnosisof inflammatory heart disease, but ithas some limitations, and weneed to be aware of those,uh, in order to beable to use the correct testto complement the, uh, CMRfindings.And the last thing, whichis, however, the most important, CMRprovides a CMR diagnosis.It does not provide anhistological diagnosis, does not provide aclinical diagnosis.So CMR provides a CMRdiagnosis that needs to put intothe clinical picture and allthings, all the features of thepatient, the clinical, the ECG,the lab test, the echo, theCMR, have to fit inone single diagnosis.And with this, I thankyou very much for your attention,and I'm happy to takeyour questions.Thank you.
Rozdziały wideo

Introduction to CMR in inflammatory myopathic cardiac syndromes
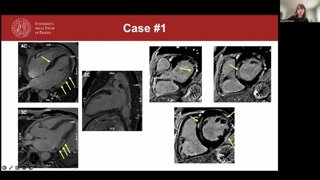
Updated Lake Louise criteria and imaging workflow
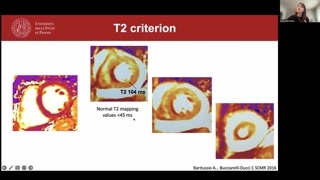
T2 imaging, edema patterns and mapping techniques

T1 mapping, extracellular volume and case review
Limitations of CMR and the role of endomyocardial biopsy

Diagnostic challenges, mapping and differential cardiomyopathy diagnosis